Knowing how to live with and care for your dialysis access is critical to helping your access stay in good health and reduce the risk for serious infection. Adjusting to life with your dialysis access may take some time, but before you know it, your daily care routine will become second nature and part of your normal everyday life. Your dialysis access plays an important role in keeping you healthy.
Here’s what you need to know about living with a dialysis access.
Tips on Caring for Your Dialysis Access
There are primarily four different types of dialysis accesses: central venous catheter (CVC), arteriovenous fistula (AV fistula), arteriovenous graft (AV graft), and peritoneal dialysis catheter (PD catheter). Each type of dialysis access has its own set of care tips and instructions that can help maintain its quality and function for as long as possible.
Caring for a CVC
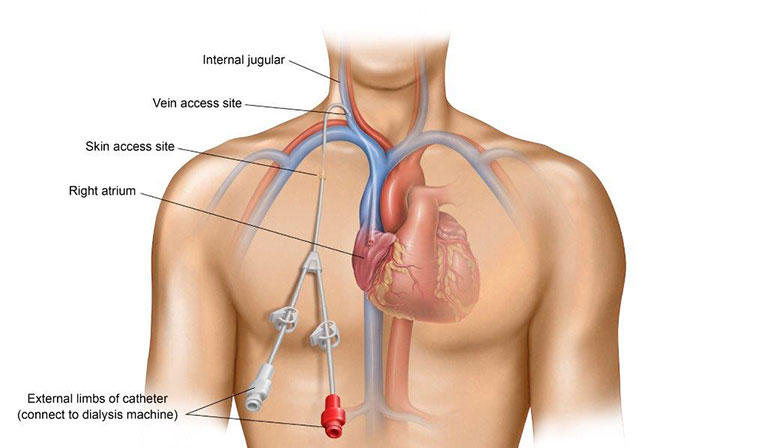 A CVC is normally used when dialysis is urgent. A CVC is a long, flexible, Y-shaped tube that is inserted through your skin into a central vein in your chest, neck, or in some situations, the groin. Your vascular specialist will instruct you on how to keep your catheter clean and intact between dialysis sessions. CVC care includes:
A CVC is normally used when dialysis is urgent. A CVC is a long, flexible, Y-shaped tube that is inserted through your skin into a central vein in your chest, neck, or in some situations, the groin. Your vascular specialist will instruct you on how to keep your catheter clean and intact between dialysis sessions. CVC care includes:
- Washing your hands thoroughly before handling your CVC if you perform dialysis at home (at a hemodialysis center, staff members will handle and care for your CVC).
- Avoiding using sharp objects, such as scissors, near your CVC.
- Keeping the CVC covered and secured to your body to prevent it from being pulled or tugged.
- Flushing your catheter once per week if you perform dialysis at home. Use a saline solution comprised of salt and water, and heparin—a drug that prevents blood clots from clogging your catheter. (i) Your dialysis care team can show you how to properly flush your catheter using these supplies (at a hemodialysis center, your catheter will be flushed and cared for by staff members.)
- Changing the dressing once per week. Be sure to wear a mask and gloves. Use alcohol pads and a cleaning solution approved by your doctor. (i)
- Keeping the dressing clean and dry always. Do not take baths or go swimming.
- Keeping the clamps on the catheter tubes always closed unless your catheter is being used. (ii)
- Looking for signs of infection every day. Signs of infection include redness, swelling, warmth, pain, fever, and discharge.
- Wearing loose, comfortable clothing that won’t get caught on your catheter.
Caring for an AV Fistula
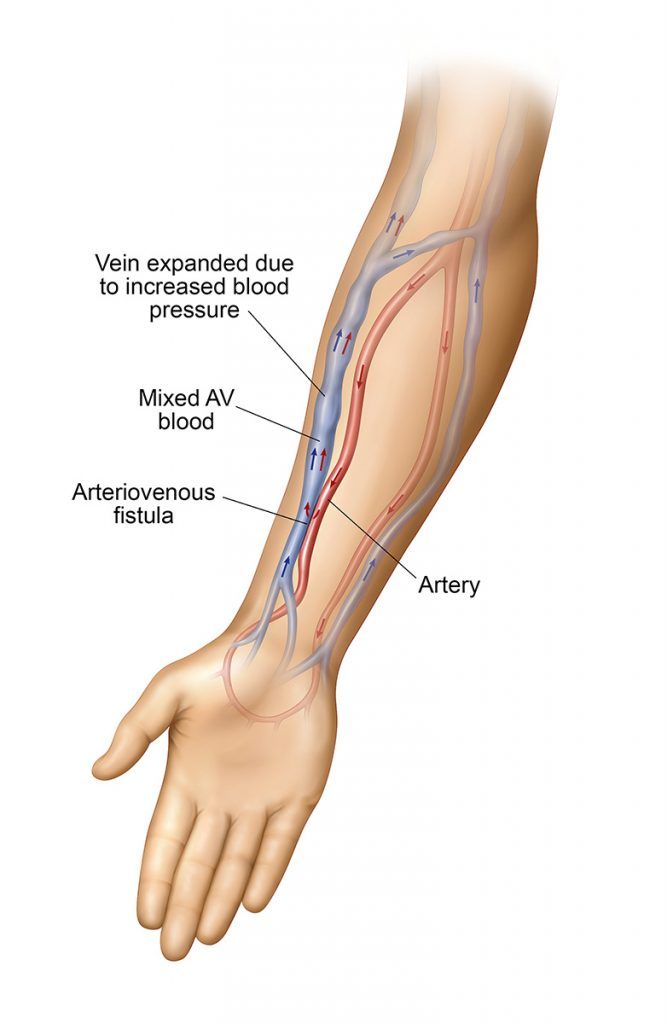 An AV fistula is the ‘gold standard’ dialysis access. An AV fistula is the connection of an artery to a vein to allow for increased blood flow and easier access to blood vessels for dialysis. (iii) A vascular specialist will usually place an AV fistula in the forearm of your non-dominant arm. An AV fistula may also be placed in your leg. AV fistula care includes:
An AV fistula is the ‘gold standard’ dialysis access. An AV fistula is the connection of an artery to a vein to allow for increased blood flow and easier access to blood vessels for dialysis. (iii) A vascular specialist will usually place an AV fistula in the forearm of your non-dominant arm. An AV fistula may also be placed in your leg. AV fistula care includes:
- Keeping your access site clean by always using antibacterial soap and water.
- Inspecting your access site every day to detect signs of infection. Signs of infection include warmth, redness, swelling, discharge, pain, and fever. (ii)
- Looking for changes in your skin that can indicate a problem with your AV fistula. Watch for signs of bleeding, peeling, and bulging.
- Listening to your AV fistula to ensure steady, proper blood flow. This can be done by putting your ear or a stethoscope to your arm or leg at the access site.
- Placing your hand or a few fingers on your AV fistula to make sure blood flow is consistent and steady. (iv) Notify your doctor immediately if you feel changes in the vibration of blood flow or feel no vibration at all.
- Avoiding putting any pressure on your access site. Do not wear tight, restrictive clothing or jewelry around the access, do not sleep on your access, and do not carry heavy bags, purses, or objects across the access. (ii)
- Not allowing anyone to draw blood from the arm or leg where your AV fistula is located.
Caring for an AV Graft
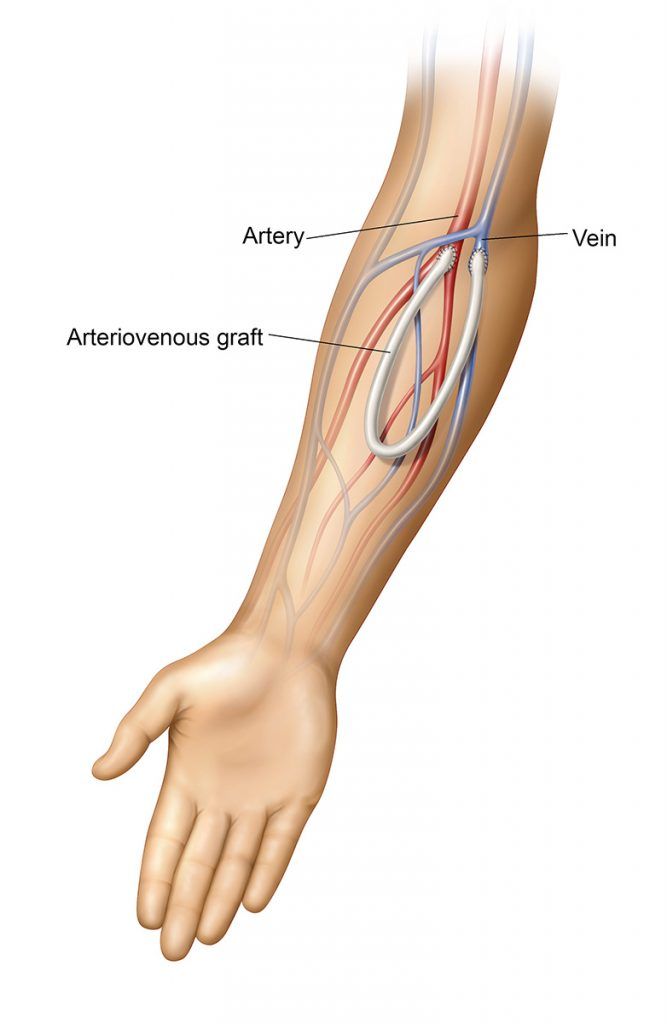 An AV graft is usually ideal for those whose veins are too small or insufficient for an AV fistula. This type of dialysis access is similar to an AV fistula, except a small, biocompatible synthetic tube is used to connect one of your arteries to one of your veins. The steps for caring for an AV graft are identical to those for an AV fistula. Keep your access site clean at all times, inspect your site daily for signs of infection, avoid putting pressure on the site, and listen and feel for steady blood flow and vibrations.
An AV graft is usually ideal for those whose veins are too small or insufficient for an AV fistula. This type of dialysis access is similar to an AV fistula, except a small, biocompatible synthetic tube is used to connect one of your arteries to one of your veins. The steps for caring for an AV graft are identical to those for an AV fistula. Keep your access site clean at all times, inspect your site daily for signs of infection, avoid putting pressure on the site, and listen and feel for steady blood flow and vibrations.
Caring for a PD Catheter
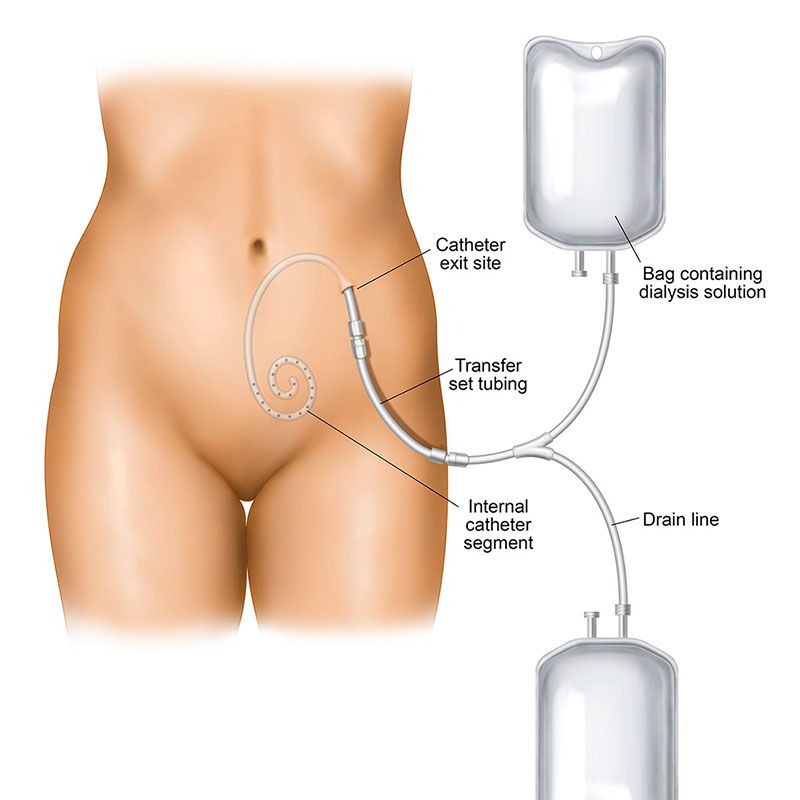 A PD catheter is used to perform peritoneal dialysis (PD), which is the process by which toxins are removed from your blood using the lining of your abdomen and a dialysate solution. This type of dialysis is linked to high risks for infection at the access site and in the tunnel where the catheter resides. PD catheter care includes:
A PD catheter is used to perform peritoneal dialysis (PD), which is the process by which toxins are removed from your blood using the lining of your abdomen and a dialysate solution. This type of dialysis is linked to high risks for infection at the access site and in the tunnel where the catheter resides. PD catheter care includes:
- Keeping your dialysis access site clean and dry and covered with a sterile dressing at all times that you are not performing a PD exchange.
- Washing your hands thoroughly using soap and water and wearing gloves before handling your PD catheter.
- Not taking baths or going swimming unless these activities are approved by your doctor. (v)
- Avoiding using sharp objects, such as scissors, near your PD catheter.
- Checking the access site every day for signs of infection. Signs of infection include redness, warmth, swelling, tenderness, and drainage.
- Not using any lotions, creams, or powder on your access site unless approved by your doctor. (v)
- Keeping your PD catheter always secured to your body to prevent it from being pulled or tugged.
- Keeping the end of the catheter always capped and closed, except when in use.
- Making sure the catheter cuff is always in place and not showing or coming out.
- Wearing loose, comfortable clothing that won’t tug or pull at your catheter.
Problems You May Encounter with a Dialysis Access
Properly caring for your dialysis access may help reduce the risk for problems. The most common problems associated with dialysis access are infection, poor blood flow, and blockage from a blood clot or scar. (iii)
Your access will be checked by your dialysis care team on a regular basis to make sure it’s working properly. Blood flow and pressure in your access may be measured, and you may undergo an imaging test called a duplex ultrasound.
Contact your nephrologist immediately if you experience any of the following:
- Redness, pain, warmth, and swelling at the access site
- Flu-like symptoms such as fever, chills, and aches (vi)
- Shortness of breath
- A temperature of 99 degrees Fahrenheit or higher (vi)
- Hearing or feeling a different sound or vibration coming from your access
- The catheter cuff on the CVC or PD catheter is showing
- Feelings of coldness, weakness, numbness, or tingling at the access site
- Blue fingers or sores at the tips of the fingers of your access arm
Call 911 or go to an emergency room immediately if you experience any of the following:
- Bleeding from an AV fistula or graft that lasts more than 20 minutes after dialysis treatment (vi)
- Any bleeding from a catheter tube or site
- A broken catheter (i)
- Absent or stopped vibration or sound from your access site
- Clogged access site
- Signs of infection
Sources:
(i) Medline Plus. (2018, September 3). Central venous catheter – flushing. Retrieved February 27, 2019, from https://medlineplus.gov/ency/patientinstructions/000157.htm.
(ii) American Kidney Fund. (n.d.). Caring for your vascular access. Retrieved February 14, 2019, from http://www.kidneyfund.org/kidney-disease/kidney-failure/treatment-of-kidney-failure/hemodialysis/caring-for-your-vascular-access.html.
(iii) National Institute of Diabetes and Digestive and Kidney Diseases. (2018, January). Hemodialysis. Retrieved February 14, 2019, from https://www.niddk.nih.gov/health-information/kidney-disease/kidney-failure/hemodialysis.
(iv) National Kidney Foundation. (n.d.). Hemodialysis access. Retrieved February 14, 2019, from https://www.kidney.org/atoz/content/hemoaccess.
(v) Fresenius Kidney Care. (n.d.). Caring for your peritoneal dialysis (PD) catheter. Retrieved February 14, 2019, from https://www.freseniuskidneycare.com/~/media/Fresenius/FKC/Tools-and-Resources/Treatment-Guides-and-Information/KCHT000541-01_PD_Catheter_Care.pdf.
(vi) National Kidney Foundation. (n.d.). Hemodialysis access: What you need to know. Retrieved February 14, 2019, from https://www.kidney.org/sites/default/files/11-50-0216_va.pdf.