Peripheral artery disease (PAD) is a common and serious condition affecting between 8 and 12 million people in the United States. PAD strikes as many as one out every twenty people who are 50 years of age or older.i However, not many people are aware of the condition that causes Peripheral artery disease, called atherosclerosis. Understanding what causes atherosclerosis and how it leads to peripheral artery disease can help patients be aware of what physical changes to look out for, when to seek medical attention and how to make effective lifestyle changes to prevent recurrence or worsening of their symptoms.
What is Atherosclerosis?
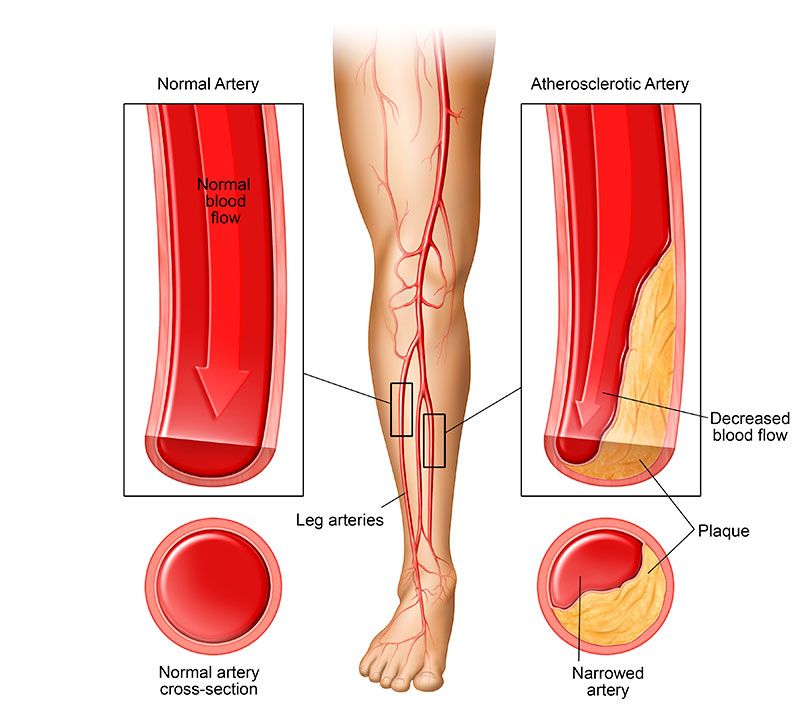
Atherosclerosis is the narrowing of the arteries caused by a buildup of plaque composed of fatty substances, calcium and cholesterol, along the interior walls of your arteries. Over time, atherosclerosis, this buildup of plaque, can cause your arteries to narrow or become completely blocked, resulting in reduced blood flow and oxygen to any artery in your body including the heart, brain, legs, kidneys and other vital organs.
The Link between Atherosclerosis and Peripheral Artery Disease
Peripheral artery disease is an atherosclerosis-related disease in which the buildup of plaque occurs in the arteries of the legs, arms and pelvis, resulting in reduced blood flow to those parts of the body. While atherosclerosis and peripheral artery disease can be common among older individuals, in addition to dialysis patients, diabetics and smokers, it is often underdiagnosed and undertreated. Symptoms of PAD include leg pain or numbness, poor nail growth on toes, and non-healing sores on toes, feet or legs. In early stages of PAD, it is possible to not have any symptoms at all.
PAD can progress slowly and worsen as you age, which is why it often goes undiagnosed. Many people attribute any symptoms they do have to simply being part of the normal aging process. Sometimes, by the time PAD is diagnosed, the damage can be so severe that limb amputation is the only treatment option available.
Risk Factors for Atherosclerosis
Although medical professionals do not know what causes atherosclerosis exactly, there are a few risk factors that can make you more prone to developing this condition. These risk factors may include. ii
- Unhealthy blood cholesterol levels
- High blood pressure
- Smoking
- Insulin resistance
- Diabetes
- Obesity
- Lack of physical activity
- Unhealthy eating habits
- Age
- Ethnicity, especially African American or Native American descent
- History of family heart disease
- High levels of protein
- Inflammation due to infection
- Low C-reactive protein (CRP) levels
- High levels of triglycerides
What are the Symptoms of PAD?
As mentioned, some people living with PAD may not experience any symptoms. One study found that 4 out of 10 patients living with PAD have no leg pain, which is typically the classic symptom.iii But as PAD progresses, some people will experience one or more of the following symptoms:
- Sores on the feet or legs that won’t heal
- Cramping or pain in the thigh or calf when walking that resolves with rest
- Fatigue
- Weakness in the arms or legs after exercise or exertion
- Loss of hair on the legs or arms
- Pale or bluish skin on the legs or arms
- Leg pain at night or while resting
- Poor toenail or fingernail growth
- Cold and painful legs or arms i
How to Treat Peripheral Artery Disease
PAD treatment begins by making the following lifestyle changes:
- Smoking cessation
- Beginning a PAD exercise regimen
- Controlling blood pressure
- Lowering cholesterol iv
If lifestyle changes alone are not enough to alleviate your symptoms and slow progression of the disease, you might be a candidate for one of three minimally-invasive treatment options:
These PAD procedures are alternatives to invasive surgery intended to reverse the effects of the narrowing caused by the plaque buildup within your arteries.
During the angioplasty procedure, your narrowed artery will be opened with a small balloon catheter. As the balloon is inflated inside the artery, it pushes the plaque build-up against the artery wall. v
During an atherectomy procedure, a special device is used to scrape and remove plaque from the walls of your arteries.vi
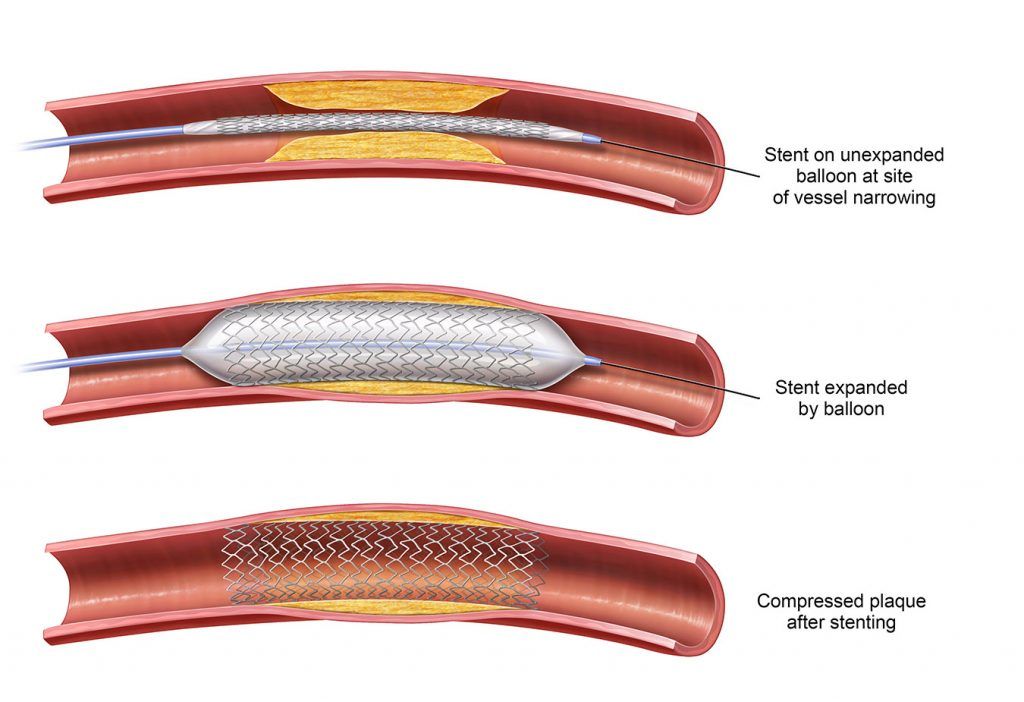
If angioplasty or atherectomy are not successful in opening your arteries and keeping them open, your doctor might elect to place a stent – a flexible, wire-mesh tube – during the angioplasty procedure. During this procedure, the stent will be permanently placed inside your artery to help hold it open. v
PAD is a serious medical condition caused by atherosclerosis requiring diagnosis and treatment to prevent major complications, including amputation or death. But with timely diagnosis and proper treatment, you can prevent PAD from progressing.
If you experience any of the symptoms of atherosclerosis or PAD described in this article, be sure to make an appointment with your doctor. There are effective treatment options to help you reclaim your lifestyle.
Sources:
i National Heart, Lung, and Blood Institute. Facts About Peripheral Arterial Disease (P.A.D.). https://www.nhlbi.nih.gov/health/educational/pad/docs/pad_extfctsht_general_508.pdf
ii National Heart, Lung, and Blood Institute (2017). Facts About Peripheral Arterial Disease (P.A.D.). Retrieved from https://www.nhlbi.nih.gov/health/health-topics/topics/atherosclerosis/atrisk
iii Ziegler?Graham K, MacKenzie EJ, Ephraim PL, Travison TG, Brookmeyer R. Estimating the Prevalence of Limb Loss in the United States: 2005 to 2050. Archives of Physical Medicine and Rehabilitation2008;89(3):422?9.
iv American Heart Association. Peripheral artery disease undertreated, understudied in women (2012, February 15). Retrieved from:
https://medicalxpress.com/news/2012-02-peripheral-artery-disease-undertreated-understudied.html
v Mayo Clinic (2017). Peripheral Artery Disease, Diagnosis and Treatment. Retrieved from: http://www.mayoclinic.org/diseases-conditions/peripheral-artery-disease/diagnosis-treatment/treatment/txc-20167509
vi Cleveland Clinic (2017). PAD Atherectomy. Retrieved from: https://my.clevelandclinic.org/health/articles/pad-atherectomy
vii Creager, M.A., Loscalzo, J. (2008) Vascular Diseases of the Extremities. In: Fauci, A.S., Braunwald, E., Kasper. D.L., et al. (eds.) Harrison’s Principles of Internal Medicine. 17th ed. New York: McGraw Hill.