If you were recently diagnosed with peripheral artery disease (PAD), your vascular specialist might have told you to watch for signs of arterial ulcers. These painful, ugly sores usually develop around the ankles and feet. PAD treatment can help reduce your risk of complications like arterial ulcers. Read on to learn more.
Causes of Arterial Ulcers
Arterial ulcers develop when there isn’t enough blood flowing to the lower legs and feet. (i) Many arterial ulcers are caused by PAD, a condition that occurs when arteries that supply blood to the legs become blocked or narrow due to atherosclerosis. (ii)
Over time, atherosclerosis, the hardening and narrowing of arteries, decreases blood flow to the legs. Reduced blood flow can affect your body’s natural healing process. Minor scrapes and leg injuries may not heal the way they should. Instead, small wounds can develop into sores. Sometimes, these sores can become badly infected. (i)
In some cases, blood flow may be blocked entirely. If your legs don’t receive enough oxygenated and nutrient-rich blood, the tissue may begin to die causing the affected area to form an open wound, or arterial ulcer. (ii)
Risk Factors for Arterial Ulcers
 Most people develop arterial ulcers due to PAD or another type of arterial blockage. (i) Some medical conditions or lifestyle factors can also increase your risk for arterial blockages. Risk factors that may contribute to the formation of an arterial ulcer are primarily those of PAD and include: (iii)
Most people develop arterial ulcers due to PAD or another type of arterial blockage. (i) Some medical conditions or lifestyle factors can also increase your risk for arterial blockages. Risk factors that may contribute to the formation of an arterial ulcer are primarily those of PAD and include: (iii)
- Smoking
- Increased age
- Obesity
- High cholesterol
- High blood pressure
- Diabetes
In addition to the PAD risk factors identified above, any injury or damage to the arteries in the legs can also create a blockage. Previous trauma to the legs, including past surgeries, may increase your risk for circulation problems. Over time, these circulation problems could lead to arterial ulcers. (iii)
What Does an Arterial Ulcer Look Like?
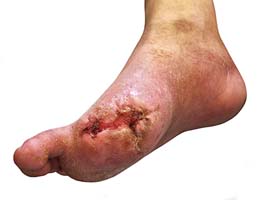
Arterial ulcers often have a hollow appearance, as if a piece of tissue has been “punched out.” These ulcers usually appear around the toes or ankles and may develop in areas of the feet where walking or poorly-fitted shoes cause extra friction. (iv)
The base of an arterial ulcer is often gray, yellow or black. Arterial ulcers can be very deep; sometimes, they even extend to the tendons or other tissues deep within the leg or foot. The skin around the arterial ulcers is often shiny, tight and dry-looking. (iv)
Arterial ulcers are often accompanied by other symptoms of PAD, including: (ii)
- Pale, cold or bluish skin
- Weak pulse in the lower legs and/or feet
- Slow-growing toenails and leg hair
Arterial Ulcers vs. Venous Ulcers
Arterial ulcers are often confused with venous ulcers. Both are vascular ulcers that result from improper circulation, but they have several differences.
Arterial ulcers develop when there isn’t enough blood flowing to the lower legs and feet. In contrast, venous ulcers develop when blood isn’t flowing from the legs back to the heart. Instead, blood backs up in the lower legs. Increased pressure inside the legs can then cause venous ulcers to form. (i)
Symptoms of these conditions can also differ. Arterial ulcers are often very painful, but venous ulcers typically cause little or no discomfort. Arterial ulcers also tend to develop around the toes and lower ankles, whereas venous ulcers develop higher up on the calves or upper ankles. (i)
Backed-up blood flow that can cause venous ulcers can also trigger swelling in the lower legs, but arterial ulcers usually don’t cause symptoms of swelling or inflammation. (i)
Can Arterial Ulcers Be Prevented?
If you suspect that you have PAD, it’s important to seek treatment as soon as possible. Although there is no cure for PAD, treatment dramatically reduces your chances of developing complications like arterial ulcers. (v)
Medications and lifestyle changes can help promote healthy blood flow to the legs. If you have significant blockages in your arteries, your vascular specialist may also recommend minimally invasive procedures to help maintain healthy blood flow in your legs and feet. (v) Proper circulation prevents arterial ulcers from developing.
It’s also essential that patients with PAD regularly inspect their legs and feet for cuts, scrapes, or sores. Taking good care of your feet can help prevent infections. (v)
If you’re concerned about the possibility of PAD and complications such as arterial ulcers, don’t delay treatment. Take our free PAD risk assessment to learn more about your risk factors for PAD and treatment options. Then call 866-LEG-DOCS (534-3627) to schedule an appointment with a vascular specialist who can help you manage your PAD and keep your legs and feet healthy for as long as possible.
Sources:
(i) Healthline. (2018, February 7). Retrieved October 24, 2018, from https://www.healthline.com/health/arterial-vs-venous-ulcers#causes
(ii) MedlinePlus. (2018, August 8). Peripheral arterial disease. Retrieved October 22, 2018, from https://medlineplus.gov/peripheralarterialdisease.html
(iii) Mayo Clinic. (2018, July 17). Peripheral artery disease: Symptoms & causes. Retrieved October 22, 2018, from https://www.mayoclinic.org/diseases-conditions/peripheral-artery-disease/symptoms-causes/syc-20350557
(iv) WoundSource. Arterial ulcers. Retrieved October 24, 2018, from https://www.woundsource.com/patientcondition/arterial-ulcers
(v) Mayo Clinic. (2018, July 17). Peripheral artery disease: Diagnosis & treatment. Retrieved October 22, 2018, from https://www.mayoclinic.org/diseases-conditions/peripheral-artery-disease/diagnosis-treatment/drc-20350563