
When you have kidney disease, dialysis can mean the difference between life and death. More than 1.5 million people around the world are treated with hemodialysis. (i) The procedure involves filtering the blood to remove wastes, extra salt and water. Many researchers and healthcare professionals agree that an arteriovenous (AV) fistula should be the first choice for an access, followed by AV graft as a second choice. However, when those access types aren’t an option, the use of a catheter for hemodialysis is necessary.
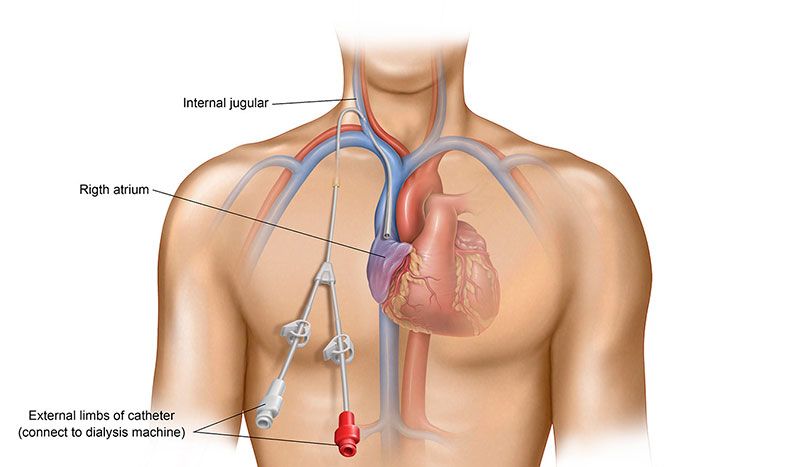
A catheter is a y-shaped tube made of soft plastic. There are two openings, one for removing your blood and the other for returning the cleaned blood to your body. It’s tunneled into place in a large vein, typically in your neck, but sometimes in your upper chest.
A hemodialysis catheter -also known as central venous catheter (CVC)– is most often used as a temporary access; however, it is also used in people who have a new AV fistula but need to start dialysis before the fistula is ready for use. Once the fistula is “mature,” the catheter is removed. In some cases, a catheter is used for a longer period if there are no other options for a permanent access such as when a patient’s blood vessels are not healthy enough for fistula creation or a graft insertion.
But what if having a catheter access for hemodialysis puts you at an equal or greater risk of illness or death? Dialysis patients who use hemodialysis catheters have a higher risk of death, infection, and heart problems than patients using other access types. Read on to learn why.
The Downside to Hemodialysis Catheters
Although some dialysis patients prefer catheters to other accesses, either because catheters don’t require needles to connect to the hemodialysis machine or because they believe their kidney function will return in a few months, catheters do pose a host of risks.
Several challenges are associated with using a central venous catheter:
- Part of the catheter is external and protrudes from your body, so it is at high risk for infections. (ii)
- Clots can form inside the opening of the catheter or form on the outside of the catheter and block the opening.
- Blood flow through a catheter may be at a lower than the blood flow rate prescribed by your doctor. (iii)
- Infection can occur even with a good blood flow rate. (iii)
- You cannot safely get a catheter wet. (iv)
Most people who need urgent hemodialysis will need a catheter to start and some dialysis patients will need one if their fistula or graft needs repair. Unfortunately, of the three main access types, catheters are most prone to infection. (iii)
The number of hemodialysis patients who have been hospitalized due to infection has increased 43 percent since 1993 and the use of dialysis catheters continues to have the largest associated risk. (v) A study reviewed 177,875 hemodialysis patients and found that patients who had a catheter were 3.8 times more likely to have an access related infection than those with an AV fistula or AV graft. (v)
Recent research found that compared with patients with fistulas, those using hemodialysis catheters had: (i)
- A 53 percent higher risk of dying.
- A 38 percent greater risk of developing a major heart problem.
- More than double the risk of developing a fatal infection.
By avoiding catheters as an initial and ongoing vascular access, h hemodialysis patients can significantly reduce their risks for death, infections and heart trouble. For patients using hemodialysis catheters, switching to a fistula or graft can diminish the heavy burden of catheter-related complications, and may save lives.
Know the Signs of Catheter Infection
Bacteria live on your skin and on environmental surfaces, so infections can occur in any kind of dialysis access. Catheters are a direct route for bacteria to get to your blood. Compared with the general population, dialysis patients have a 100-fold higher risk of sepsis-related death, with infection-related deaths highest in those with catheters. (iii)
The warning signs of an infection include: (ii, iii)
- Swelling
- Fever
- Chills
- Pus, other discharge or drainage from the catheter exit site
- Redness or tenderness around the catheter exit site
- A general feeling of weakness and illness
Regardless of access type, if you’re on dialysis and experience any of these symptoms, call your doctor or dialysis care team immediately.
For more information, download Understanding Your Dialysis Access or call 866-996-9729 to schedule an appointment with a vascular specialist.
Sources:
(i) Ravani, P., Palmer, S. C., Oliver, M. J., Quinn, R. R., Macrae, J. M., Tai, D. J., . . . James, M. T. (2013). Associations between hemodialysis access type and clinical outcomes: A systematic review. Journal of the American Society of Nephrology,__24(3), 465-473. doi:10.1681/asn.2012070643
(ii) Medical Education Institute, Inc. (n.d.). Vascular Access for Hemodialysis. Retrieved October 1, 2018, from https://lifeoptions.org/living-with-kidney-failure/vascular-access/
(iii) Napalkov, P., Felici, D. M., Chu, L. K., Jacobs, J. R., & Begelman, S. M. (2013). Incidence of catheter-related complications in patients with central venous or hemodialysis catheters: A health care claims database analysis. BMC Cardiovascular Disorders, 13(1). doi:10.1186/1471-2261-13-86
(iv) Fresenius Kidney Care. (n.d.) Hemodialysis catheter. Retrieved November 30, 2018, from https://www.freseniuskidneycare.com/ckd-treatment/types-of-dialysis-access.
(v) Lok, C. E., & Foley, R. (2013). Vascular access morbidity and mortality: Trends of the last decade. Clinical Journal of the American Society of Nephrology, 8(7), 1213-1219. doi:10.2215/cjn.01690213


