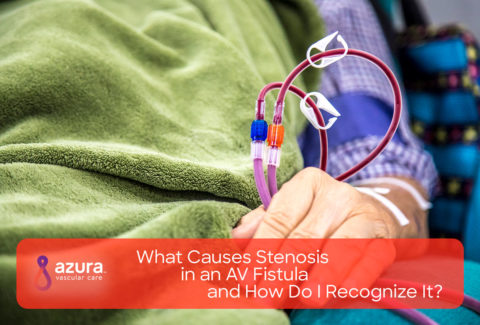
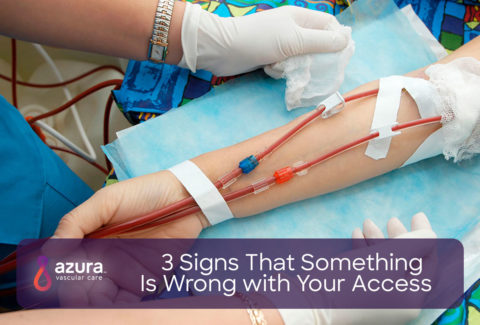
If you’re one of the 700,000 people in the United States needing dialysis, you’re at risk of developing a clot in your dialysis access, regardless of the type of access you may have. If this happens, you need to receive treatment as soon as possible because with a clotted dialysis access, you will not be able to receive your next hemodialysis treatment until the access is either repaired or replaced.
Why Does Blood Clot During Dialysis?
There are two main ways a dialysis access can become clotted, or blocked:
- stenosis
- thrombosis
What is Stenosis?
Stenosis is when a blood vessel narrows. It’s a common cause of access dysfunction, particularly with arteriovenous (AV) fistulas and AV grafts. Stenosis in any vein or artery can create changes in blood flow and pressure throughout the dialysis access. (2)
A narrowing of an artery that feeds your AV fistula or graft can slow the flow of blood through your access during treatment. If the blood flow is significantly reduced, it can lead to inadequate dialysis, and is quite likely to cause the access to become totally blocked or clotted.
If the stenosis occurs on the venous side of your dialysis access, the narrowed vein will result in a backup in pressure and blood flow prior to the stenosis. If the stenosis is significant enough in size it may completely block off the blood flow through your fistula or graft.
In either of the above situations, once the blood flow through the fistula or graft has stopped, it means that your access has thrombosed (the medical term for ‘clotted’).
What is Thrombosis?
If thrombosis occurs in your AV fistula or AV graft, blood flow will be reduced or even prevented from moving through your access. A blood clot can also occur in a central venous catheter (CVC). Regardless of where a thrombosis occurs, it needs to be treated as soon as it’s discovered. (2)
3 Treatments for A Clotted Access
- Tissue Plasminogen Activator
- Thrombectomy of an AV fistula or AV graft
- Catheter-Directed Thrombolysis
Tissue Plasminogen Activator
The first step in treating a clotted CVC is the administration of a “clot busting” medication called tissue plasminogen activator (tPA). In some cases, this can be adminnistered in the dialysis center. If this doesn’t work, you might need to be referred to an access center for a vascular specialist to evaluate why the CVC has clotted. There are several methods that the vascular specialist may use to attempt the declotting of your CVC. If these methods are unsuccessful, you may need to have your catheter replaced. (1)
Thrombectomy of an AV fistula or AV graft
A thrombectomy is a catheter-guided procedure to remove the blood clot. Our specially trained physicians at Azura Vascular Care perform this outpatient procedure to remove the clot from the fistula or graft by using an instrument specifically designed to do so, eliminating the need for a more invasive procedure.
For the thrombectomy procedure, a local anesthetic to numb the area first will be administered and if needed, a moderate sedative may be given to help you relax. A vascular specialist will insert a catheter into your dialysis access guided by X-ray technology. The catheter is used to break up and remove the clot. In some cases, a specialized instrument will be inserted through the catheter to aid in breaking up and removing the clot. The catheter is removed when the clot has been retrieved and the procedure is complete. This procedure efficiently removes the clot and restores blood flow. The procedure takes about an hour and no overnight stay is required.
Catheter-Directed Thrombolysis
Thrombolysis, also known as thrombolytic therapy, is the use of drugs as treatment for the breakdown (lysis) of blood clots that have blocked your dialysis access. This treatment involves the injection of clot-busting drugs through a catheter which deliver drugs directly to the site of the blockage. The goal of this clot busting procedure is to restore blood flow through your access.
Thrombolysis is a minimally invasive, outpatient procedure performed by a vascular specialist. For the procedure, you will first be given a local anesthetic to numb the area and if needed, a moderate sedative to help you relax.
Then, using X-ray technology to guide a catheter into your clotted access, a clot dissolving medication will be delivered through the catheter directly to the blood clot. Once the medication has been delivered to the affected area, it will be left to dwell for a period of time to break up the clot. Removal of the clot from the vessel by thrombolysis is a relatively quick procedure (usually completed in less than one hour). At the end of the procedure, the catheter used to perform the procedure is removed.
If your access clots, it’s important that you seek treatment as soon as possible. Keeping your access free of clots means you’ll be able to rest easy, trusting your access is functioning properly so that you’re getting the life-saving dialysis treatments you need.