Approximately one in five adults will develop varicose veins at some point in their lives. (i) If you are one of the many millions of people with this common vein condition, you may be planning to seek vein treatment. Managing varicose veins successfully requires planning and a big part of that planning means taking advantage of windows of opportunity. This includes everything from optimizing insurance coverage to choosing the best time to treat varicose veins.
4 Reasons Why Fall is the Best Time to Start Varicose Veins Treatment
1. Fall weather conditions make wearing compression stockings more comfortable
Compression stockings are a common treatment option for varicose veins. These special stockings fit snugly and help blood flow through your vessels, which can lessen the pain and swelling associated with varicose veins. (ii)
Many insurance companies require a conservative treatment protocol, such as wearing compression hose for a specified period of time, before other procedures are covered.
No one enjoys wearing compression socks during the warmer months. Fall, on the other hand, is the optimal time to feel cozy in compression stockings.
2. Fall brings cooler weather for optimal healing
During pre- and post-operative periods, heat and ultraviolet (UV) rays should be avoided. Heat causes veins to dilate, which may cause blood to pool in dysfunctional veins. UV rays can break down the collagen in the layers of the skin, which causes the skin to lose elasticity and weaken vein walls. During the fall season, UV rays begin to drop off substantially in several locales. (iii)
3. Fall often coincides with insurance coverage cycles or turnover
Often insurance coverage starts anew in January. When you begin your treatment in the fall, insurance usually turns over just in time for treatment—or surgery if warranted—following pre-operative treatments. Insurance turnover is especially important if you have a yearly cap. (iv) Also, if you begin treatment before the end of the year, you may have already met your insurance deductible, which may mean less out-of-pocket costs. Beginning your assessment in the fall can mean a great outcome to start the New Year.
4. Fall treatment prepares legs for warmer weather
Beginning treatment in the fall also helps prepare your legs for the following summer when it’s warm enough to forgo long pants and opt for shorts and bathing suits. With vein treatment, you may need more than one session to notice positive results. After treatment, it may take up to several weeks for full healing.
This is just one more reason that the best time to treat varicose veins is in the fall.
Varicose Veins: What You Need to Know
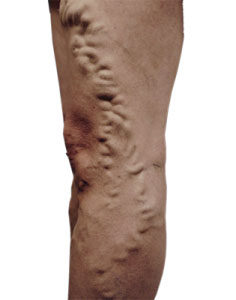
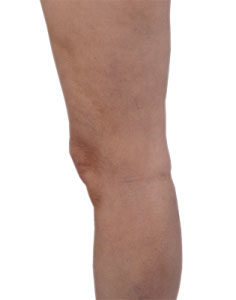
Statistics show approximately 73 percent of all women and 56 percent of men suffer from varicose veins. (v) Depending on the level of severity, these veins can be virtually unnoticeable or unsightly—bluish or purple cords, twisted and sometimes protruding.
Occasionally, body weight and skin shade can mask early symptoms, and leg changes are attributed to something else—weight gain, lack of exercise, a normal part of aging—but left untreated, varicose veins can cause: (vi)
- Leg dermatitis – This skin condition results in redness, swelling, and blistering. Dermatitis caused by untreated varicose veins can be particularly hard to treat because the source of the dermatitis is ongoing.
- Leg changes – These changes can include a heavy feeling in the legs, achy legs, lower leg swelling and burning. You might also notice increased leg pain after movement or during prolonged standing. Discoloration and itching, especially near the ankles, is another early symptom.
- Superficial thrombophlebitis – This means that blood clots have formed in smaller leg veins. This is not a dangerous situation, but it is painful and can have a significant impact on quality of life.
- Venous skin ulcers – These are open sores that form on your legs, especially near the ankles. When varicose veins are left untreated, these ulcers are slow to heal—often taking months—because the underlying cause of the ulcers is ongoing. Venous skin ulcers can become infected, which may lead to potentially serious complications.
- Bleeding – Untreated varicose veins can burst and cause swelling and substantial leg pain.
Varicose Veins Increase Risks for Complications
A comprehensive study published earlier this year found that varicose veins significantly increase the risks for life-threatening complications, including: (vii)
- Deep vein thrombosis and pulmonary embolism – This is a far more serious condition than superficial thrombophlebitis. In deep vein thrombosis, a blood clot forms in a vein deep in the body—most often in the lower leg or thigh. A deep vein thrombosis has the potential to break away and travel to the lung, causing a pulmonary embolism, which is often fatal.
- Peripheral artery disease– This is a common circulatory problem in which narrowed arteries reduce blood flow to your limbs.
Avoiding these complications is crucial for long-term mobility, pain management, and quality of life.
Managing Varicose Veins
Managing varicose veins goes back to taking advantage of windows of opportunity—choosing the best season to begin assessment and treatment—but successful treatment also calls for lifestyle changes in conjunction with treatment management.
According to the National Heart Lung and Blood Institute, there are a few things you can do to optimize your treatment results and help prevent new varicose veins from forming:
- Avoid sitting or standing for long periods.
- Move your legs often, including exercising to keep blood flowing.
- If you are overweight, try losing weight to take pressure off your legs.
- Avoid tight clothing that restricts blood flow below the waist.
If you are considering varicose veins treatment this fall, or if you would like to schedule an appointment with a vascular specialist, call 866.996.9729 today.
Sources:
(i) PubMed Health. Varicose Veins: Overview. Accessed October 9, 2018, from https://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0072431/.
(ii) Kakkos, S.K., Timpilis, M., & Patrino P. (2018). Acute effects of graduated elastic compression stockings in patients with symptomatic varicose veins: A randomised double blind placebo controlled trial. European Journal of Vascular and Endovascular Surgery, 55(1):118-125.
(iii) Sun Safety Monthly Average UV Index. Environmental Protection Agency. Accessed September 25, 2018, from https://www.epa.gov/sunsafety/sun-safety-monthly-average-uv-index.
(iv) Annual Limits. Healthcare.gov. Accessed September 25, 2018, from https://www.healthcare.gov/glossary/annual-limit/.
(v) Davies, M.G., Lumsden, A.B. (2011) Chronic venous insufficiency. Minneapolis: Cardiotext Publishing, LLC.
(vi) Varicose Veins. National Heart, Blood and Lung Institute. Accessed September 25, 2018, from https://www.nhlbi.nih.gov/health-topics/varicose-veins.
(vii) Chang, S.L., Huang, Y.L., Lee, M.C., Hu, S., Hsiao, Y.C., Chang, S.W., … Chen, P.C. (2018) Association of varicose veins with incident venous thromboembolism and peripheral artery disease. JAMA 319(8):807-817.