If you’ve been diagnosed with diabetes, you probably already know you need to take care of your feet. Your doctor has likely told you to pay particular attention to any non-healing foot cuts or sores you notice. And then it happens: one day you may be looking down and find yourself wondering “how long has that sore been there?”
What Is a Non-Healing Foot Ulcer?
What are diabetic foot ulcers? Diabetic foot ulcers are wounds present on the foot or below the ankle, which do not heal. The presence of these ulcers is a leading cause of amputation due to diabetes.[i] The Centers for Disease Control and Prevention estimates that about 73,000 lower-limb amputations, not related to trauma, are performed every year on people with diabetes.[ii]
This is why if you’re living with diabetes and have a sore, or an open area, on your foot that:
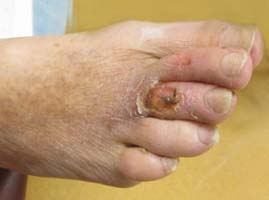 doesn’t appear to be healing
doesn’t appear to be healing- is red
- is hot to the touch
- is draining pus
- or just keeps coming back
you may have a non-healing diabetic foot ulcer, and should make an appointment with your doctor as soon as possible.
Non-Healing Foot Ulcers and Peripheral Artery Disease (PAD)
Foot Ulcers may be a sign that you may have peripheral artery disease (PAD). PAD develops when the build up of plaque in the arteries of the limbs, typically the legs, decreases the amount of blood and oxygen getting to your legs and feet. It’s estimated that 50% of people living with diabetes and non-healing foot ulcers also have PAD.[iii]
How Foot Ulcers Develop
Ulcers begin with an injury or an irritation to the foot. Even a seemingly small injury, such as a splinter in the foot, stepping on a tack, or a blister from a shoe, can lead to an ulcer if you have diabetes or PAD.
The following conditions make the development of an ulcer more likely:
Diabetic neuropathy is one of the most common complications of diabetes, as well as one of the leading causes of diabetic foot ulcers.[iv]
- Diabetic neuropathy results from damage to the nerves in the arms and legs. You may notice either tingling or the loss of feeling in your feet. Neuropathy usually:
- begins in the toes
- occurs on both sides
- progresses up the legs
- Neuropathy can also change how you use your feet to walk and, over time, this can lead to changes in the actual shape of your feet. These changes increase your risk for ulceration as well.
- Up to 60% of ulcerations in people living with diabetes are thought to be related to diabetic neuropathy alone.[iv]
RELATED: 5 Reasons Why You Have Developed a Non-Healing Foot Ulcer
PAD results from a blockage of blood supply to the legs. This is a serious condition, particularly if there is an injury, because the necessary oxygen and blood needed to heal an injury may not be able to reach the ulcer.
About 45% of ulcers are due to the presence of both PAD and neuropathy.[iv]
Symptoms of PAD can include:
- Pain or fatigue in the leg when walking that tends to get better with rest
- Non-healing foot ulcers
- Leg pain at rest
- Toes, feet or legs that are pale or blue in color
- One leg is cooler to the touch than the other
- Decreased leg hair growth
- Decreased toenail growth
The Consequences of Waiting – Possible Outcomes
If you think you have a diabetic foot ulcer, you need to see your doctor right away to determine if you have PAD. The infection increases the demand for oxygen in that area, but, if you have PAD, the blood vessels may not be able to deliver the oxygen needed and the infection will probably worsen.
Your physician can conduct testing to determine if the ulcer is resulting from PAD and treatment options can then be determined. Bypass graft surgery may be one option, as is non-surgical angioplasty. Angioplasty is minimally invasive and can be performed to improve the blood flow to the ulcer and encourage healing, but only if PAD is diagnosed early enough. The longer you wait to treat PAD, the more likely it is that the ulcer could ultimately lead to amputation as the only treatment option.
If you’re concerned that you have a non-healing diabetic foot ulcer, you need to see your doctor. Your doctor can examine your foot and determine the next step in treatment with the goal of avoiding amputation.
If you suspect you have PAD, discuss the need for further evaluation with your doctor to determine if poor blood flow is preventing the healing of your diabetic foot ulcer.
Sources:
[i] American Diabetes Association. Consensus Development Conference on Diabetic Foot Wound Care: 7-8 April 1999, Boston, Massachusetts. American Diabetes Association. Diabetes Care. 1999;22:1354-1360.
[ii] Centers for Disease Control and Prevention. National Diabetes Statistics Report: Estimates of Diabetes and Its Burden in the United States, 2014, Atlanta, GA: US Department of Health and Human Services; 2014. http://www.cdc.gov/diabetes/data/statistics/2014statisticsreport.html (accessed 8/1/2016)
[iii] Brownrigg, J.R.W., Apelqvist, J., Bakker, K., Schaper, N.C., and Hinchliffe, R.J., Evidence-based management of PAD & the Diabetic Foot. Euro J Vasc and Endovasular Surg, 2013. 45(6): p. 673-681. http://www.ejves.com/article/S1078-5884(13)00136-6/abstract (accessed 7/30/2016)
[iv] Boulton AJ, Kirsner RS, Vileikyte L. Clinical practice. Neuropathic diabetic foot ulcers. N Engl J Med. 2004;351:48-55.
[v] Bartus CL, Margolis DJ. Reducing the incidence of foot ulceration and amputation in diabetes. Curr Diab Rep. 2004;4:413-418.
[vi] Boulton AJ, Vileikyte L, Ragnarson-Tennvall G, Apelqvist J. The global burden of diabetic foot disease. Lancet. 2005;366:1719-1724