I think I may have a diabetic foot ulcer – what should I do?
What are diabetic foot ulcers?
Should I be concerned?
If you’ve thought about any of these questions, it may be time to consider talking to your doctor.
Diabetic foot ulcers are sores on the feet or anywhere below the ankle that someone with diabetes may develop. If you have diabetes and you have an open sore on your foot that just won’t heal, is red, painful, and warm, is draining pus, smells funny or just doesn’t seem to get better, then you may have a non-healing diabetic foot ulcer.
If this is you, you need to see your doctor as soon as possible to discuss your options for treatment.
Diabetic foot ulcers are common – in fact, 1 in 4 people with diabetes will develop at least one ulcer post-diagnosis.[i] Ulcers can be serious and life threatening; they are the leading cause of amputation due to diabetes. If you want to avoid a foot amputation due to diabetes, it’s important to have your foot ulcer evaluated by your doctor.
What Are Diabetic Foot Ulcers?
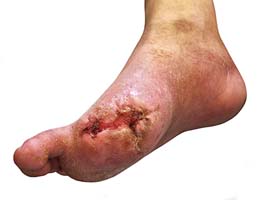 Diabetic foot ulcers generally begin with an injury to the foot. This injury can come from stepping on a tack, a small cut from dry skin or even just a blister from a shoe that doesn’t fit correctly. In someone without diabetes, these types of injuries would typically heal on their own. For people living with diabetes, this is not always the case.
Diabetic foot ulcers generally begin with an injury to the foot. This injury can come from stepping on a tack, a small cut from dry skin or even just a blister from a shoe that doesn’t fit correctly. In someone without diabetes, these types of injuries would typically heal on their own. For people living with diabetes, this is not always the case.
What Causes Diabetic Foot Ulcers?
Here are some conditions that increase the likelihood of an ulcer forming in a patient with diabetes:
Diabetic neuropathy – Diabetes can cause damage to nerves in parts of the body, particularly the feet. It’s one of the most common complications experienced by people living with diabetes.[i] This damage to the nerves can alter sensation in the feet, resulting in anything from increased sensitivity and pain to tingling and complete loss of sensation.
Peripheral artery disease (PAD) – This comes from a blockage of the arteries in the legs. When someone has PAD, blood vessels are not able to deliver the oxygen and nutrients needed for an ulcer to heal. Around 45% of diabetic foot ulcers occur in people who have both diabetic neuropathy and PAD.[i] Some symptoms of PAD include:
- Pain in the legs due to activity – pain usually improves with rest
- Pain in the legs even while at rest
- Legs that get tired with activity
- Decreased growth of leg hair or toenails
- One leg or foot that is cooler than the other
- Toes or a foot that is pale or blue in color
- Non-healing foot ulcer
There are effective treatments for PAD that may restore blood flow and relieve symptoms and help ulcers heal.
Other Factors – Other conditions that increase the likelihood of having a diabetic foot ulcer may include:
- Being male
- Being older than 60 years of age
- Abnormal shape of the foot, either due to prior amputation or other ulcer on the feet
- Problems seeing well
- Chronic kidney disease
- High blood sugar measurements[i]
Are Ulcers Life Threatening?
An ulcer alone is not life threatening. However, if the ulcer is untreated, eventually, it can become life threatening, especially in cases of:
- Infection – Bacteria can get into the body through the ulcer. Any ulcer that’s present for more than 30 days is at increased risk for infection.[ii] Bacteria can cause a serious infection in the tissue that can get into the blood stream and cause a life threatening condition known as sepsis. The infection can also spread, causing a bone infection known as osteomyelitis. If left untreated, osteomyelitis can also lead to sepsis. Certain kinds of bacteria can cause necrotizing fasciitis, a very aggressive infection that can lead to death.
 Ischemia – If PAD is present, then tissue can die due to lack of blood flow. Dead tissue, or gangrene, if left untreated, can become infected and lead to death.
Ischemia – If PAD is present, then tissue can die due to lack of blood flow. Dead tissue, or gangrene, if left untreated, can become infected and lead to death.- Amputation – It may seem strange to say that amputation, which is a treatment for a foot ulcer, can be life threatening. But a person with diabetes who has had an amputation has a much higher risk of mortality than a non-amputee.[iii]
Don’t Wait
It’s important to take a diabetic foot ulcer seriously. Waiting longer than 6 weeks to seek treatment for an ulcer may mean it’s more likely that it won’t heal.[iv] Ulcers have a better chance of healing if they’re cared for by a specialized team which can include a diabetes specialist, a wound specialist, a foot specialist, an infectious disease specialist, and a vascular specialist, such as a vascular surgeon or interventional radiologist.[v]
There are effective treatments for foot ulcers that are designed to avoid amputation due to diabetes. If you seek treatment early, you will increase the likelihood that your ulcer may heal. If you have PAD, there are treatments that can increase the blood flow and further promote healing. Set up an appointment to see your doctor today if you have a diabetic foot ulcer that is not yet being treated.
Sources:
[i] Amin, N., and Doupis, J., Diabetic foot disease: From the evaluation of the “foot at risk” to the novel diabetic ulcer treatment modalities. World J Diabetes, 2016. 7(7): p 153-164. http://www.wjgnet.com/1948-9358/full/v7/i7/153.htm (accessed 7/30/2016)
[ii] Lipski, B.A., Berendt, A.R., Cornia, P.B., Pile, J.C., Peters, E.J., Armstrong, D.G., Deery, H.G., Embil, J.M., Joseph W.S., Karchmer, A.W., Pinzur, M.S., Senneville, E., 2012 Infectious Disease Society of America clinical practice guideline for the diagnosis and treatment of diabetic foot infections. Clin Infect Dis, 2012, 54(12): e132-73. https://www.guideline.gov/summaries/summary/37220/2012-infectious-diseases-society-of-america-clinical-practice-guideline-for-the-diagnosis-and-treatment-of-diabetic-foot-infections (accessed 8/11/2016)
[iii] Brownrigg, J.R.W., Apelqvist, J., Bakker, K., Schaper, N.C., and Hinchliffe, R.J., Evidence-based managed of PAD & the Diabetic Foot. Euro J Vasc and Endovasular Surg, 2013. 45(6): p. 673-681. http://www.ejves.com/article/S1078-5884(13)00136-6/abstract (accessed 7/30/2016)
[iv] Margolis, D.J., Allen-Taylor, L., Hoffstad, O., Berlin, J.A., Diabetic Neuropathic Foot Ulcers. Diabetes Care, 2002, 25(10): p. 1835-1839. http://care.diabetesjournals.org/content/diacare/25/10/1835.full.pdf (accessed 8/4/2016)
[v] Weck, M., Slesaczeck, T., Paetzold, H., Muench, D., Nanning, T., von Gagern, G., Brechow, A., Dietrich, U., Holfert, M., Bornstein, S., Barthel, A., Thomas, A., Koehler, C., and Hanefeld, M., Structured health care for subjects with diabetic foot ulcers results in a reduction of major amputation rates. Cardiovascular Diabetology, 2013, 12: article 45. http://cardiab.biomedcentral.com/articles/10.1186/1475-2840-12-45 (accessed 8/4/2016)